🚨 SHE LEFT FOR A HAIR APPOINTMENT ON A RAINY DAY… ONE RED LIGHT LATER, HER LIFE WAS FOREVER CHANGED. 😢💔
Five weeks ago, 16-year-old Dilynn Turner stepped out into the Alabama rain, excited for fresh highlights and a normal teen afternoon. Then, at one fateful red light, everything shattered in a violent crash. Traumatic brain injury. Fractured skull. Brain bleed. Broken bones. Doctors once said she might not make it — her family braced for the worst.
Now, at Shepherd Center in Atlanta, she’s fighting inch by inch: relearning how to swallow (she just chewed and swallowed ice — a massive win), moving her head to look around, grimacing in pain (a sign she’s feeling more), even glancing toward her parents with that fragile spark of awareness.
Her mom’s raw updates hit hard: “Progress comes in inches… and every inch is celebrated.” But the road is long — up to two years for her brain to reach its new potential. Is she truly coming back? What small miracle will happen next?
Latest emotional update — her mom’s words, the tiny victories, and why hope feels so fragile yet so real. Grab tissues. 👇
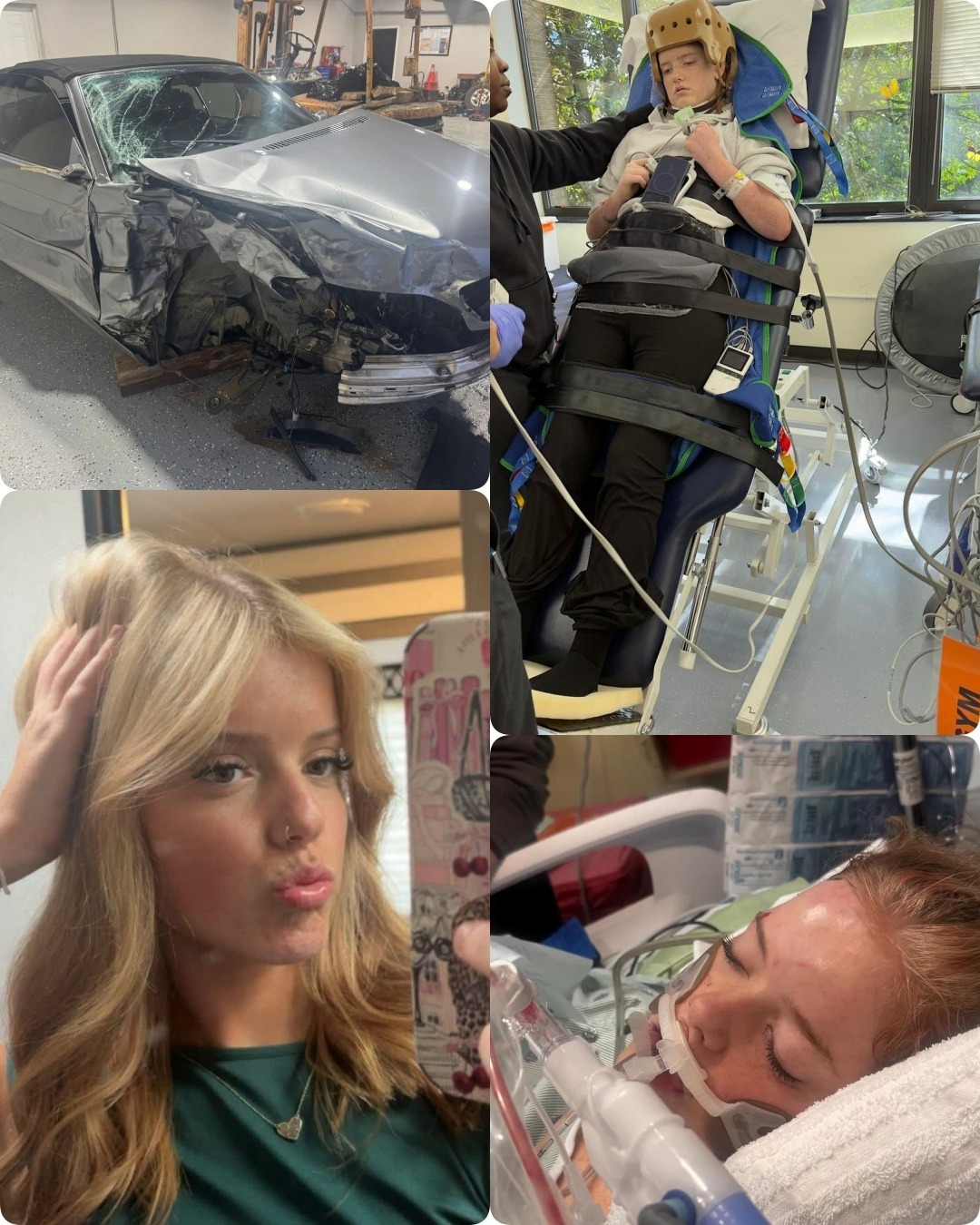
Five weeks after a rainy-day car accident altered the course of her young life, 16-year-old Dilynn Turner continues intensive rehabilitation at Shepherd Center in Atlanta, one of the nation’s premier facilities for brain and spinal cord injury recovery. What began as a routine trip for a hair appointment on November 5, 2025, ended in a high-impact collision at a red light, resulting in traumatic brain injury (TBI), skull fractures, brain bleeding, a broken leg, broken jaw, ruptured ear, and other injuries that initially placed her life in grave danger.
Dilynn, a junior at Good Hope High School, was transported to local hospitals before stabilizing enough for transfer to Huntsville Hospital, where neurosurgeons performed a bilateral decompressive craniectomy to relieve dangerous brain swelling. Family members, including mother Jessica Methvin, have shared that early days were marked by uncertainty — at one point, her prognosis was so dire that medical staff, including her neurosurgeon, showed visible emotion during discussions.
Now, approximately five weeks post-accident (around mid-December 2025 into early 2026 updates), Dilynn has been at Shepherd Center for several weeks, participating in daily regimens of physical, occupational, and speech therapy. Progress, as described by her mother and relayed through local media and social media channels, remains incremental but meaningful in the context of severe TBI.
Recent family updates highlight several milestones:
Dilynn has demonstrated the ability to chew and swallow small amounts, such as ice, after opening her mouth to accept it. Medical explanations note that post-TBI, the brain can temporarily “forget” automatic functions like swallowing due to disrupted neural pathways. Relearning these skills indicates reconnection in critical areas of the brain, with implications for future speech and oral motor control.
She expresses discomfort through facial grimacing and vocal moans — signs of increased awareness and sensory processing.
During tilt-table sessions (a therapy tool that gradually brings patients to upright positions), Dilynn has held her head mostly unassisted for short periods and turned it to look around, tolerating upright positioning for hours at a time to aid circulation, breathing, and neurological re-patterning.
She has tolerated a speaking valve on her tracheostomy for longer durations, a step toward potential verbal communication, though timing of vocal cord opening remains inconsistent.
Brief glances toward family members and responses to stimuli, including phone calls from friends played near her, have been noted as encouraging signs of emerging awareness.
Jessica Methvin has been candid in updates shared via platforms monitored by local reporters, such as Cullman Daily News and journalist Rick Karle. In one recent message, she described a medical conference with Dilynn’s doctor: the physician reviewed scans, the extent of initial injury, current status, and long-term outlook. While acknowledging the severity — recovery could take up to two years to reach “new full potential” — he expressed measured optimism about ongoing healing and neuroplasticity.
Dilynn remains in a minimally conscious to semi-conscious state much of the time, with periods of increased wakefulness interspersed with significant fatigue and sleep needs. Therapy sessions challenge her to stay engaged, and setbacks like pain (possibly from surgical sites or headaches related to craniotomy) or muscle tightness requiring interventions such as Botox have been addressed by her multidisciplinary team.
The accident’s circumstances remain limited in public detail, with reports indicating it occurred at a red light during rainy conditions. No further information on other vehicles, fault determinations, or legal proceedings has been widely released, as the focus has stayed on medical recovery rather than investigation.
Shepherd Center’s specialized approach includes structured daily schedules, family involvement, and emphasis on functional gains over timelines. Dilynn’s ability to tolerate wheelchair positioning for extended periods supports respiratory and circulatory health while her brain re-adapts to upright posture. Occupational therapy targets fine motor skills and daily living activities, while speech-language pathologists work on swallowing safety and potential communication tools.
Community response in Cullman County and beyond has been substantial. A GoFundMe organized by Jessica Methvin has helped cover medical and travel expenses, with donors contributing amid widespread prayers and messages of support. Local media have amplified family updates, turning small victories — like head control or swallowing — into shared moments of hope.
Medical experts consulted in similar cases emphasize that severe TBI recovery varies widely. Initial swelling and secondary injuries can cause lasting changes, but consistent therapy leverages the brain’s ability to form new connections. Swallowing progress, in particular, is viewed as a foundational step, reducing risks like aspiration pneumonia and opening pathways for nutrition and speech.
For Dilynn’s family — including father Derek, stepfamily members, and siblings — each day brings a mix of exhaustion and gratitude. Jessica has described the emotional toll of watching her daughter relearn basics once taken for granted, yet highlighted the “spark” in fleeting glances or efforts that remind them Dilynn is still present and fighting.
As Dilynn continues inpatient rehab, the emphasis remains on patience and persistence. Doctors reiterate no firm guarantees, but incremental gains — an inch of head movement, a swallow of ice, a turn toward her parents — fuel ongoing hope. In a journey measured not in days but in tiny, hard-won steps, Dilynn Turner’s resilience has become a focal point for her community and supporters following her story.
The family continues to request prayers for pain management, brain healing, muscle relaxation, and endurance through therapy. With each fragile advance, they hold onto the possibility that their daughter — once headed for a simple hair appointment — will reclaim more of herself in the months and years ahead.
News
Royta Giles Jr.: 8-Year-Old Killed by Stray Bullet in 2020 Riverchase Galleria Shootout While Shopping for Fourth of July Clothes
🚨 HE WAS JUST AN 8-YEAR-OLD EXCITED FOR FOURTH OF JULY CLOTHES… STANDING IN LINE WITH MOM AT THE MALL….
Heidi Miller: The 4-Year-Old Sole Survivor of 2016 Amtrak Train Crash That Claimed Her Family on Way to Church Near Trinidad, Colorado
🚨 THEY WERE ALL DRESSED UP FOR CHURCH… ONE UNGATED CROSSING LATER, ONLY A 4-YEAR-OLD LITTLE GIRL SURVIVED TO ASK…
‘Hero’ Teen Jordan Everett Died Trying to Save Friend Joshua Myers from Oncoming Train at Poynton Station, Inquest Rules
🚨 ONE TEEN JUMPED ON THE TRACKS IN DESPAIR… HIS BEST FRIEND RUSHED TO SAVE HIM — AND BOTH WERE…
Cassidy Stay: The Lone Survivor of 2014 Texas Family Massacre Who Played Dead After Being Shot in the Head
🚨 SHE OPENED THE DOOR FOR A “FEDEX GUY”… AND WATCHED HER ENTIRE FAMILY GET EX3CUTED ONE BY ONE. THEN…
Phoenix Movers and QuikTrip Guard Credited with Rescuing 2-Year-Old Kehlani Rogers After Amber Alert Abduction from Avondale Home
🚨 ORDINARY MOVERS BECOME REAL-LIFE SUPERHEROES IN SECONDS… SAVING A 2-YEAR-OLD FROM A KIDNAPPER RIGHT IN FRONT OF THEM! 😱🚚💪…
Abel Mwansa: A 12-Year-Old’s Life Cut Short in Tumbler Ridge Mass Shooting, Leaving a Legacy of Kindness Across Continents
🚨 A 12-YEAR-OLD BOY LEFT HOME FOR SCHOOL… AND NEVER CAME BACK. HIS NAME NOW ECHOES ACROSS TWO CONTINENTS. 😢🇨🇦🇿🇲…
End of content
No more pages to load












